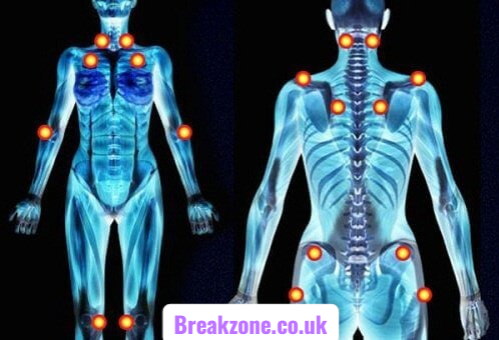
Inomyalgia refers to persistent or recurring muscle pain that can result from inflammation, muscle strain, nerve sensitivity, or underlying health conditions. Common symptoms include soreness, stiffness, fatigue, and reduced mobility. Diagnosis generally involves a physical examination and a review of medical history, while treatment may involve rest, gentle exercise, pain management strategies, and lifestyle adjustments. Early intervention and preventive habits can help reduce discomfort and support long-term muscle health.
Muscle discomfort can impact daily activities, movement, and overall well-being, making it important to understand its causes and management. This guide explores the meaning, causes, symptoms, and treatment approaches for inomyalgia in a practical and accessible way. It highlights how lifestyle factors, stress, physical strain, and medical conditions contribute to muscle pain, and provides safe strategies to support recovery and prevention. By combining medical insights with everyday wellness guidance, this article empowers individuals to make informed decisions about caring for their muscles, improving mobility, and maintaining a healthier, more active lifestyle.
Understanding the Medical Meaning and Broader Context of Persistent Muscle Pain
Muscle pain is a common experience that ranges frommild soreness after activity to ongoing discomfort that interferes with routine movement. Inomyalgia is often discussed in relation to inflammation, strain, or nerve sensitivity affecting muscle tissue. Recognizing the broader medical context helps individuals understand why discomfort appears without obvious injury. Awareness also supports timely care, preventing minor irritation from progressing into chronic tension or mobility limitations that influence posture, sleep quality, and overall physical balance in everyday life.
How Muscle Structure, Nerves, and Circulation Contribute to Pain Sensations
Healthy muscles rely on coordinated nerve signals, oxygen-rich blood flow, and balanced tissue repair. When any of these systems become disrupted, aching or stiffness may develop. Poor circulation can limit nutrient delivery, while irritated nerves may amplify pain signals beyond the original source. Structural stress from overuse or sudden movement further increases sensitivity. Understanding these internal processes clarifies why muscle discomfort sometimes persists even after visible strain disappears, highlighting the importance of recovery, hydration, and gradual physical conditioning.
Common Lifestyle and Physical Triggers That Lead to Ongoing Muscle Discomfort
Daily habits strongly influence muscular comfort. Long hours of sitting, repetitive motion, poor posture, and insufficient stretching often create tension that accumulates gradually. Sudden intense exercise without preparation can also stress fibers and surrounding connective tissue. Emotional stress contributes by tightening muscles unconsciously, especially in the neck, shoulders, and back. Recognizing these triggers allows individuals to adjust routines, incorporate movement breaks, and maintain balanced activity levels that protect muscle function over time.
The Role of Inflammation and Immune Response in Muscle Tenderness Development
Inflammation is a natural healing response, yet excessive or prolonged inflammation may increase soreness and sensitivity. Immune activity releases chemical signals that attract repair cells to affected tissue, sometimes causing swelling or warmth. When this response becomes persistent, discomfort may continue beyond the initial injury. Nutrition, rest, and gentle mobility influence how efficiently inflammation resolves. Supporting the body’s recovery processes can shorten healing time and reduce the likelihood of lingering muscular irritation.
Recognizing Early Warning Signs Before Pain Becomes Chronic or Limiting
Early symptoms often appear subtly, including mild stiffness, fatigue after light activity, or localized tenderness when pressing on muscle areas. Ignoring these signals may allow tension patterns to deepen, reducing flexibility and strength. Paying attention to posture, sleep quality, and movement comfort helps identify concerns before they intensify. Prompt self-care and professional guidance when needed can prevent progression toward persistent discomfort that affects daily independence and long-term physical resilience.
Diagnostic Approaches Doctors Use to Evaluate Persistent Muscle Conditions
Healthcare professionals typically begin with detailed medical history and physical examination to understand symptom patterns, activity levels, and possible injuries. They may assess range of motion, strength, and areas of tenderness. In some cases, imaging or laboratory testing helps rule out underlying disorders affecting muscles or nerves. Accurate evaluation ensures treatment targets the true source of discomfort rather than only masking symptoms, supporting safer and more effective recovery.
Also read this: Antarvwsna Meaning, Emotional Depth, Cultural Context, and Personal Growth
Evidence-Based Treatment Strategies That Support Safe Muscle Recovery
Treatment commonly focuses on relieving pain while restoring normal movement. Gentle stretching, gradual strengthening, and adequate rest allow tissues to heal without excessive strain. Supportive therapies such as heat application or relaxation techniques may reduce tension and improve circulation. When necessary, healthcare providers guide additional care suited to individual needs. Consistent, balanced recovery methods are essential for preventing repeated irritation and maintaining comfortable mobility.
The Importance of Movement, Flexibility, and Gradual Strength Building
Regular physical activity keeps muscles nourished, flexible, and resilient. Slow progression in exercise intensity helps fibers adapt safely, reducing the risk of strain. Flexibility training maintains joint range and prevents stiffness that can contribute to discomfort. Balanced strengthening supports posture and distributes physical load evenly across the body. Sustainable movement habits are one of the most reliable ways to protect long-term muscular health and reduce recurring pain episodes.
How Stress, Sleep Quality, and Emotional Health Influence Muscle Tension
Mental and emotional states directly affect physical tension. Stress hormones encourage muscle tightening, while poor sleep limits tissue repair and increases pain sensitivity. Relaxation practices, consistent sleep routines, and emotional support can therefore improve muscular comfort alongside physical treatments. Addressing both mind and body creates a more complete recovery environment, reducing the cycle of tension and fatigue that often accompanies persistent discomfort.
Nutritional Factors That Support Muscle Repair and Energy Balance Naturally
Muscles depend on adequate protein, hydration, vitamins, and minerals to repair microscopic strain and maintain strength. Insufficient nutrition may slow healing or increase fatigue, making soreness feel more intense. Balanced meals and steady fluid intake support circulation and tissue recovery. Thoughtful nutritional habits complement physical therapy and movement, forming a foundation for sustainable muscular wellness without extreme or restrictive approaches.
Preventive Habits That Reduce Recurrence of Inomyalgia in Daily Life
Prevention centers on consistent posture awareness, regular stretching, moderate exercise, and stress management. Small routine adjustments, such as ergonomic seating or scheduled movement breaks, can significantly reduce strain accumulation. Listening to the body’s signals and responding early prevents minor tension from becoming persistent discomfort. Long-term prevention is often simpler and more effective than repeated treatment after pain develops.
Differences Between Temporary Muscle Soreness and Persistent Pain Disorders
Short-term soreness after unfamiliar activity usually improves within days as muscles adapt. Persistent pain lasting weeks or recurring frequently may indicate deeper imbalance or underlying conditions. Distinguishing between these patterns guides appropriate care and prevents unnecessary worry. Awareness encourages timely consultation when symptoms extend beyond normal recovery, ensuring safe and informed health decisions.
When Professional Medical Advice Becomes Important for Safety
Medical guidance is essential when pain is severe, long-lasting, or accompanied by weakness, numbness, or limited movement. Early evaluation helps identify treatable causes and prevents complications. Seeking help is a proactive step toward recovery rather than a sign of weakness. Professional support ensures that care strategies remain safe, personalized, and aligned with overall health needs.
Long-Term Outlook and Quality-of-Life Improvements Through Consistent Care
With proper management, most individuals experience meaningful improvement in comfort, strength, and flexibility. Gradual lifestyle adjustments often provide lasting relief and support active living. Consistency remains the key factor, as muscles respond best to steady care rather than sudden changes. A proactive approach transforms recovery into ongoing wellness that benefits the entire body.
Conclusion: Building Sustainable Muscle Health Through Awareness and Action
Understanding inomyalgia helps individuals identify symptoms early, address underlying causes, and adopt habits that promote lasting comfort. By combining medical guidance with daily self-care, a balanced approach to recovery and prevention becomes possible. Incorporating movement, proper nutrition, stress management, and timely professional support can significantly improve long-term muscle health. Regular attention to the body’s needs supports enhanced mobility, reduced discomfort, and a more active, confident, and fulfilling lifestyle.
FAQs (People Also Ask)
What is inomyalgia?
It describes ongoing or recurring muscle pain often linked to inflammation, strain, or nerve sensitivity affecting muscle tissue.
What causes persistent muscle pain without injury?
Poor posture, stress, overuse, inflammation, and certain medical conditions can all contribute to continuing discomfort.
How is muscle pain diagnosed?
Doctors evaluate symptoms through physical examination, medical history, and sometimes imaging or laboratory tests.
Can lifestyle changes improve muscle discomfort?
Yes, regular movement, balanced nutrition, proper sleep, and stress reduction often reduce pain and support recovery.
When should someone see a doctor for muscle pain?
Medical advice is important if pain is severe, lasts several weeks, or includes weakness or numbness.
Is gentle exercise safe during recovery?
Gradual, low-impact movement usually helps healing by improving circulation and flexibility.
Can muscle pain return after treatment?
Recurrence is possible if underlying habits or stressors remain, which is why prevention strategies are important.
Fore more info: Breakzone.co.uk